Understanding the Role of Denial in Addiction

Denial is a complex psychological mechanism that plays a significant role in the development, maintenance, and treatment of addiction. For individuals struggling with substance use disorders and their loved ones, understanding denial is crucial for recognizing the need for help and taking steps towards recovery. At Destination Hope, we recognize the importance of addressing denial […]
Is Vyvanse Addictive?
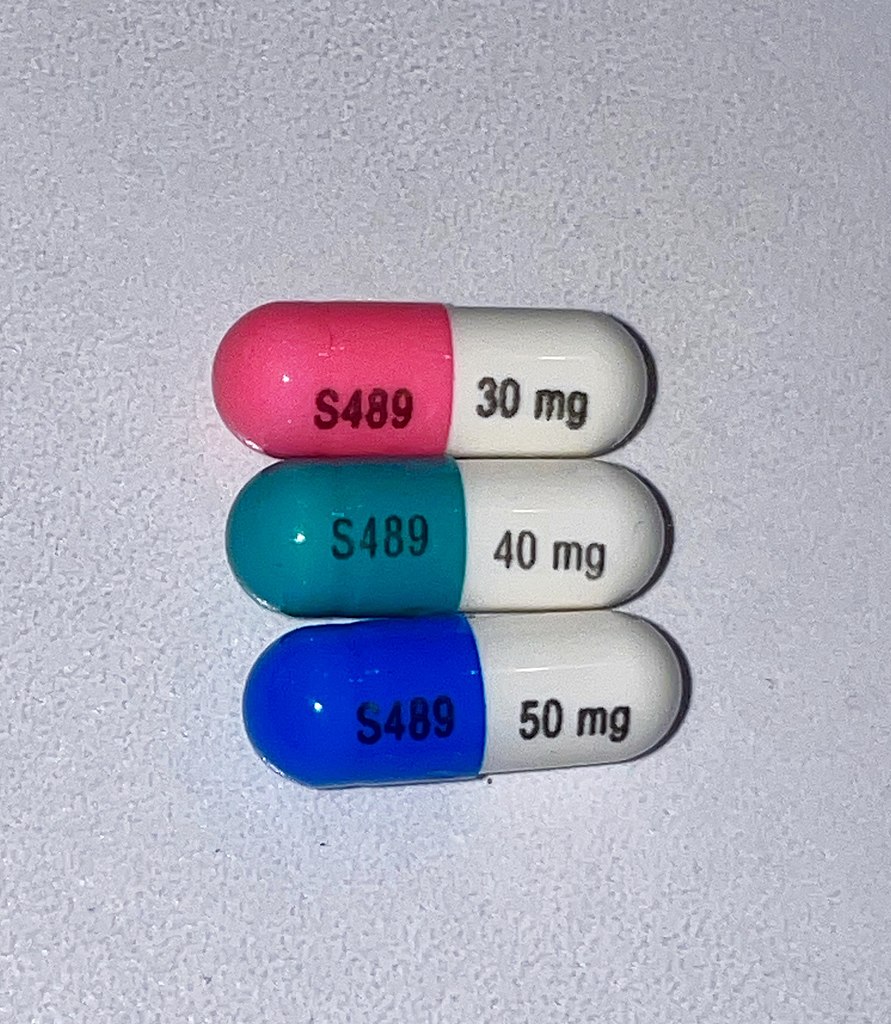
Vyvanse, a prescription medication used to treat attention deficit hyperactivity disorder (ADHD) and binge eating disorder, has gained popularity in recent years. However, with its increasing use comes the question: is Vyvanse addictive? As a stimulant medication, Vyvanse carries the potential for abuse and addiction, making it crucial for individuals to understand the risks associated […]
Can Xanax Make Anxiety Worse?

Discover the unexpected effects of Xanax as we explore the question, “Can Xanax make anxiety worse?” Unravel the concept of paradoxical reactions to this medication and understand the potential causes behind increased anxiety.
Helping a Loved One with Alcoholism

Discover effective strategies to support someone struggling with alcoholism in this comprehensive blog. Learn about communication, emotional support, treatment options, boundaries, and self-care.
How Does Alcohol Affect Serotonin: Understanding the Relationship
Discover the impact of alcohol on serotonin levels in the brain in this informative blog. Learn about the short-term and long-term effects on mood and mental health.
Can Drugs Cause Mental Health Disorders?

Explore the intricate connection between drug use and mental health disorders. Understand how drugs can trigger or exacerbate mental health conditions, and the complex factors that contribute to this relationship.
What Is Cross Tolerance In Addiction?

Addiction is a complex issue that can manifest in multiple ways.
How to Help Someone with Drug Addiction and Depression

If you intend to someone with addiction and depression, it’s important to approach the situation with compassion, understanding, and patience. It can be difficult to open up about addiction and depression, so it’s important to give them a safe space to talk without judgment. Try not to let your own anxiety or worry lead you […]
International Overdose Awareness Day: Get Involved
International Overdose Awareness Day has been observed since it was founded in Australia in 2001. Overdose, both fatal and non-fatal, is one of the world’s worst and most baffling public health crises. It occurs when the body ingests more of a drug, including alcohol, than it can process, leading to an overload of its systems. […]
How to Speak to Your Employer about Addiction
If you have recently returned to work after attending a rehabilitation program, or are beginning a new position, it is important that your employer understands the position you are currently in (if you feel comfortable speaking to them about it). Not only will having a discussion with your employer about your addiction help you understand […]
